My name is Jennie and I’ve have been working for Central and North West London (CNWL) Camden NHS for 10 years now. I’ve recently moved from a clinical role as an occupational therapist into a project role where I am setting up a telehealth service. I want to let you know how the service operates.
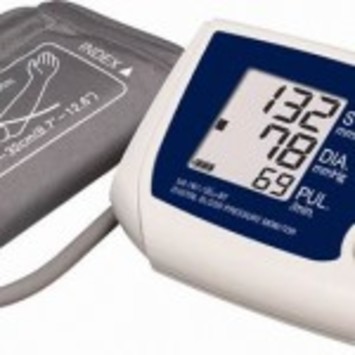
Telehealth equipment uses technology to monitor a patient’s health on a daily basis. The simple to use devices check blood pressure, heart rate, weight and oxygen levels to help identify any changes. This can help to manage their condition better, such as identifying to the patient when they need to take it easy or when it’s time to contact the contact the doctor.
The results are automatically transmitted to the community telehealth triage team who will monitor them each day (Monday to Friday). If they have any concerns they will contact the patient and may arrange for a healthcare professional to visit them at home. If the patient has any concerns they can still contact their healthcare professional to discuss. But if they feel unwell they should contact their GP, or 111 or 999 in a medical emergency as the service is not available on Saturday or Sunday (or bank holidays).
Telehealth is a small electronic device that is connected to the telephone line in the home. There are also devices available that wirelessly transmit the readings if a telephone line is unavailable. As well as gathering biometric information, the devices will also ask questions about general health and well-being, such as ‘do you have a cough? do you have any other symptoms related to your cough? Do you need a clinician to call you?’
If any abnormal readings are identified a healthcare professional will make contact with the patient to discuss any action that needs to be taken.
Many telehealth users say the equipment gives them confidence and peace of mind to manage their condition at home. It can help them understand more about their condition and how it can be affected. Family and friends also find telehealth gives reassurance and confidence that the patient’s condition is under control.
The service can make a real difference to quality of life as any signs of ill-health can be picked up at an early stage so that they can be treated quickly, before symptoms get worse. We have based our project on the department of health’s; Whole System Demonstrator’ randomised control trial and will be comparing their outcomes with ours. The people using telehealth in the trial demonstrated the following when compared to the control group
- 15 per cent reduction in Accident and Emergency
- 20 per cent reduction in emergency admissions
- 14 per cent reduction in elective admissions
- 14 per cent reduction in bed days
- 45 per cent reduction in mortality rates.
We will be leasing 25 telehealth units as of the 14 of July 2014 for a one year period. Initially the units will be prescribed by the CNWL Camden clinicians working within the respiratory and heart failure teams to patients with Chronic Obstructive Pulmonary Disease (COPD) and/or heart failure.
Launch event
We are running a drop in launch event on 30 July between 2-5pm at The Groves Lounge, 2nd Floor South Wing, St Pancras Hospital, 4 St Pancras Way, London NW1 0PE.
No need to confirm attendance, just pop in to find out more and trial the equipment
For more information, or to discuss if a patient may be suitable to use telehealth then contact me [email protected] 020 3317 3387.